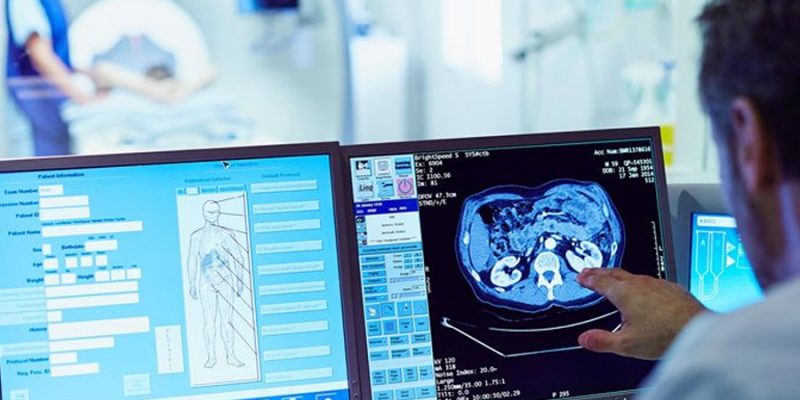
Artificial intelligence is crucial for the healthcare industry, but market failure prevents healthcare AI software diffusion.
It should not be surprising that artificial intelligence (AI) technology and the machine learning sector are still in their early stages of development given the complexity of the healthcare industry. We’re just not there yet; expecting the market to be farther advanced would be like expecting a kid who can perform one-digit addition to also be able to do calculus.
In a recent STAT+ article titled “A market failure is preventing efficient diffusion of healthcare I software,” the authors present a case for why the adoption of AI software in the field of healthcare is still relatively low and discuss what the sector can do to advance the technology’s incorporation into clinical decision support capabilities.
Given the complexity of the healthcare business, it should not come as a surprise that machine learning and artificial intelligence (AI) technology are still in their early phases of development. Expecting the market to be more developed would be like expecting a child who can complete one-digit addition to also be able to conduct calculus. We’re just not there yet.
The authors of a recent STAT+ article titled “A market failure is preventing efficient diffusion of healthcare I software” argue why adoption of AI software in the medical field is still comparatively low and go over what the industry can do to advance the technology’s integration into clinical decision support capabilities.
Second, while the authors distinguish between fixed and variable costs associated with adopting and using Artificial intelligence, they stop short of really quantifying the costs associated with implementing artificial intelligence on a per-unit or per-instance basis. Additionally, they don’t evaluate the worth of artificial intelligence or the benefits to society in relation to the expenditures, which makes such a compensation scheme all but impossible.
Third, even though having governance and quality assurance for artificial intelligence is crucial—many coalitions and public-private partnerships have been formed precisely for this reason—the authors fail to provide any examples of the harm that might result from a lack of artificial intelligence adoption. (One presumes that this is due, among other things, to the difficulty of currently establishing and quantifying damage in the context ofhealthcare, as well as the dearth of cases indicating advantages.)
Unfortunately, using government incentives as a policy vehicle does not work well for more recent innovations and unproven business models. One may observe the foolishness of such an undertaking by looking at recent experience, which the STAT writers also mention.
The EHR Incentive Program (a component of HITECH) had an unforeseen consequence, according to the STAT+ authors, in that “EHR companies transformed this windfall of taxpayer cash into a barrier to entry,” which they then exploit to market their own artificial intelligence products. They don’t appear to be thinking about the possibility that a different federal incentive scheme may provide a bonanza for artificial intelligence providers that create their own entry barriers.
The federal government is really peculiarly ill-suited to manage such an incentive scheme as new advancements in the application of artificial intelligence in healthcare emerge and lessons are learned. Though it is too large to fail, it moves too slowly to keep up with the rate of artificial intelligence advancement. It is best to leave individual fake intelligence firms and healthcare systems to deal with such unavoidable commercial failures, technological advancements, and lessons learned.
E-prescribing is maybe the finest illustration of well-implemented subsidized uptake of health IT. Beginning in 2009, federal incentives to encourage e-prescribing adoption were a resounding success; by 2010, 40% of doctors who had adopted had done so as a direct result of the program. Due in large part to the fact that e-prescribing was an established technology, standards were in place to ensure interoperability between doctors and pharmacies, there was already an ecosystem and network infrastructure in place, and studies had been conducted proving the benefits, the market and competitive landscape for e-prescribing grew.
Health IT adoption is not something that can, or should, be handled by a policy intervention alone – especially when a technology is this immature, as the $35B failure of the EHR incentives program confirms.
There may be functions that the government can do. As an industry convener, it may bring together professionals from business, technology, and academia to inform government bodies and offer standardized suggestions for handling the technical and policy problems that artificial intelligence developers and implementers deal with. By linking incentives to reimbursement, the government, which through CMS is the country’s largest payer, can promote adoption once standards are established and use cases have shown their value. Alternatively, by using value-based payment systems more frequently itself, the government can foster the conditions necessary for health systems to adopt artificial intelligence that has been shown to enhance outcomes and quality of care.



















